Quarterly
provincial
review
meetings
and
clinic
audits
repeatedly
flag
this
trend,
prompting
the
city’s
health
leaders
to
sound
the
alarm.
In
an
interview
with
CITE,
Bulawayo’s
Provincial
Medical
Director
(PMD),
Dr
Maphios
Siamuchembu
said
the
trend
is
as
baffling
as
it
is
dangerous.
“I
would
estimate
between
one
percent
and
five
percent
of
our
patients,
give
us
this
problem.
One
thing
that
happens
is
people
feel
better
and
they
think,
‘I
don’t
need
to
continue
this
treatment.’
But
that’s
not
the
case,”
said
Dr
Siamuchembu.
“Patients
think
they’re
cured”
–
the
PMD’s
warning
The
PMD
said
treatment
of
TB
takes
a
minimum
of
six
months
while
treatment
of
HIV
is
lifelong.
“When
you
interrupt
that,
you’re
basically
culturing
resistance
and
it
comes
back
stronger
then
we
have
no
arsenal
to
treat
you,”
he
said.
“You
get
a
patient
who
is
admitted
to
Thorngrove
Hospital,
he
has
drug-resistant
TB
but
then
they
abscond.
They
jump
over
the
fence
of
the
hospital,
and
they
disappear.”
He
said
the
health
system
itself
is
not
blameless
as
it
has
limited
security
at
facilities
where
some
patients
literally
evade
care,
even
though
nurses
make
follow
ups
to
patients’
houses.
“You
enter
the
gate
and
they
ask
who’s
there.
You
say,
‘it’s
the
health
workers,
we
want
to
find
out
about
your
medicines.’
They
say
‘wait
for
me
outside,
and
then
they
jump
the
durawall,”
he
said.
“Some
pitch
up
months
later
in
a
worse
condition.
And
you
wonder
why
people
do
that,
because
as
far
as
we’re
concerned,
we’re
trying
to
help
them
get
better,
and
also
to
control
that
they
don’t
spread
TB
to
other
people.”
Siamuchembu
said
defaulters
often
give
false
names,
phone
numbers
and
addresses.
“We
call
their
phone
numbers
they’ve
given
us
and
it
says
this
one
does
not
exist.
We
follow
up
at
the
address
and
we
are
told,
‘we
don’t
know
this
person.’
Then
we
can’t
find
them,
and
we’re
worried
because
this
person
is
not
on
treatment.
As
you
interrupt
treatment,
these
diseases
become
worse.
It’s
a
huge
problem.”
A
hidden
threat
amid
years
of
progress
The
PMD
said,
“I
am
not
happy
with
any
defaulter.”
From
United
Bulawayo
Hospitals
(UBH)
to
Mzilikazi,
Njube
and
Nketa,
health
workers
are
recording
case
after
case
of
patients
who
vanish
mid-treatment,
often
resurfacing
only
when
critically
ill
or
not
at
all.
In
a
recent
provincial
health
TB
review
meeting
in
the
first
quarter
of
2025
(Q1
2025),
health
officials
admitted
bluntly
that
they
have
“inadequate
knowledge
on
factors
contributing
to
high
Lost
To
Follow-Up
(LTFU)
rate”
so
they
must
“conduct
operational
research
on
factors
contributing
to
high
LTFU
in
the
city.”
Defaulting
or
being
“lost
to
follow-up”
(LTFU)
in
clinical
language
is
not
just
a
statistical
headache
but
a
threatening
challenge
that
can
undo
hard-won
progress
in
containing
two
of
Zimbabwe’s
deadliest
epidemics
–
TB
and
HIV
in
Bulawayo.
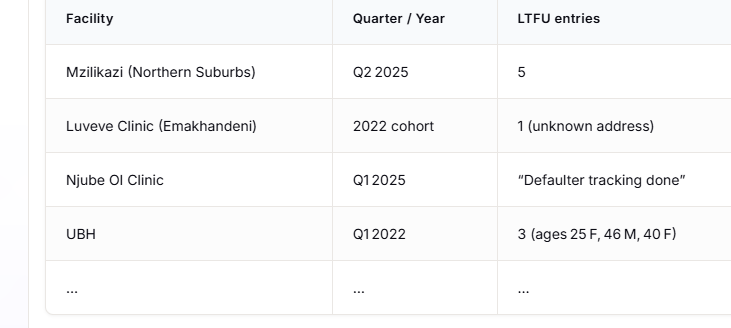
Looking
at
minutes
from
quarterly
provincial
review
meetings
and
clinic
audits,
here
are
some
of
the
cases
documented
‘when
patients
disappear.
From
numbers
to
faces
The
data
is
not
abstract.
Individual
stories
illustrate
the
human
cost.
A
25-year-old
woman
had
been
stable
on
antiretroviral
therapy,
but
stopped
coming
for
reviews
after
seven
months.
The
staff
tried
to
call
her,
then
checked
the
address
she
had
given
but
it
drew
a
blank.
Her
file
now
reads:
LTFU
at
seven
months.
She
is
not
the
only
one.
In
the
same
cohort,
a
46-year-old
man
dropped
out
at
month
eight,
and
a
40-year-old
woman
at
22
months.
All
had
given
unreachable
contacts.
At
Nketa
Clinic,
a
TB
death
audit
was
described
as
a
“very
ill
patient…
ART
defaulter.”
In
other
words,
failing
to
take
HIV
treatment
had
left
the
patient
fatally
vulnerable
when
TB
struck.
The
data
reviewed
by
CITE
shows
a
persistent
pattern
across
Bulawayo’s
three
administrative
districts
–
Emakhandeni,
Nkulumane
and
the
Northern
Suburbs,
where
clinic
registers
show
loss
to
follow-up.
A
glimpse
of
the
data
shows
these
are
not
isolated
cases
but
are
symptomatic
of
a
system
where
patients
slip
through
cracks.
Together,
these
records
show
a
clear
pattern,
patients
dropping
out
of
either
HIV
or
TB
treatment
in
different
clinics,
over
the
years
and
across
districts.
The
broader
epidemiological
picture
According
to
the
2025
HIV
Estimates
Report
for
Bulawayo
Metropolitan,
as
of
2024,
an
estimated
76
608
people
were
living
with
HIV
in
the
province.
This
represents
a
decrease
from
79
711
recorded
in
the
2020
Zimbabwe
Population-based
HIV
Impact
Assessment
(ZIMPHIA),
after
calibration
for
more
accurate
population
estimates.

Although
this
signals
a
cautiously
optimistic
outlook
for
Bulawayo,
health
officials
continue
to
address
challenges
such
as
treatment
defaulting
and
follow-up
gaps
that
threaten
to
undermine
these
achievements.
Data
from
Mpilo
Hospital
(Jan–Aug 2025)
A
fresh
analysis
of
Mpilo
Hospital’s
outpatient
infectious
disease
register
for
the
first
eight
months
of
2025
highlights
a
troubling
divide
in
adherence
to
ART.
The
data
reveals
stark
differences
between
patients
who
briefly
abandon
treatment
and
those
who
disappear
entirely
from
the
system.
According
to
the
hospital
records,
73
individuals
who
missed
appointments
eventually
returned
to
care,
classified
as
“Back‑to‑Care.”
In
contrast,
378
patients
are
listed
as
LTFU,
having
had
no
contact
with
the
clinic
for
six
months
or
more.
For
every
patient
who
re-engages,
more
than
five
slip
through
the
cracks.
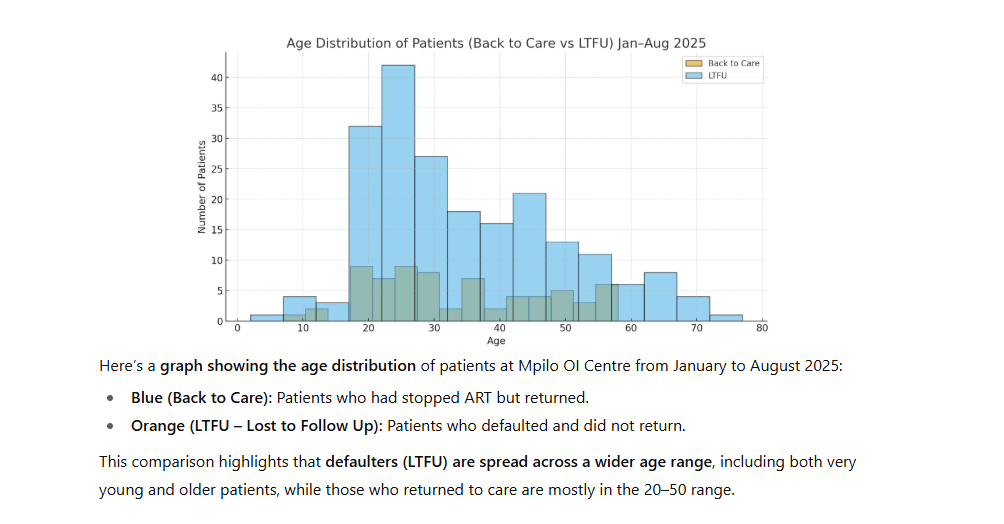
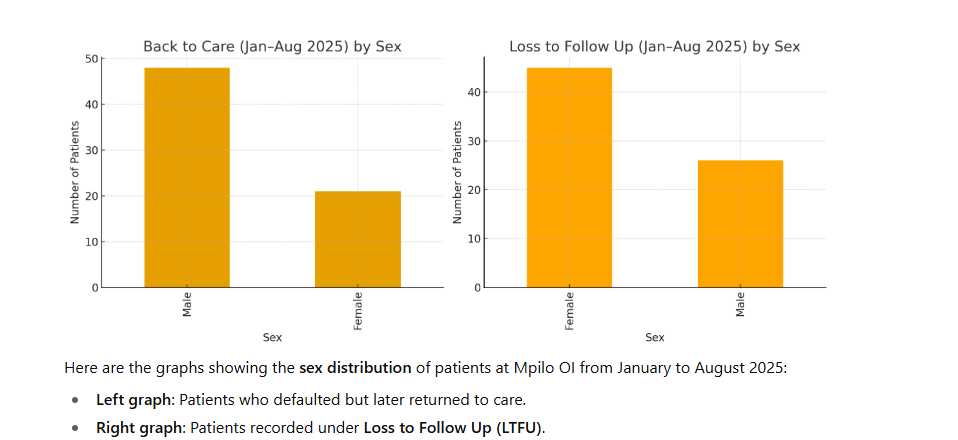
The
demographic
profile
shows
a
predominantly
youthful
cohort
in
their
twenties,
which
may
mean
many
are
juggling
school,
work
and
family
responsibilities
alongside
the
demands
of
daily
medication.
Gaps
for
back-to-care
patients
ranged
from
under
a
month
to
nearly
four
years,
though
40
percent
of
returns
occurred
within
six
months
of
the
missed
visit.
LTFU
gaps,
by
definition,
exceed
six
months,
a
sizeable
proportion
extends
beyond
a
year
and
a
few
cases
stretch
past
three
years,
indicating
chronic
disengagement.
Short
interruptions
were
far
more
likely
to
be
resolved,
while
prolonged
absences
sharply
reduced
the
likelihood
of
re-engagement,
particularly
for
patients
on
second‑line
or
more
complex
regimens.
Most
patients
returning
to
care
were
still
on
first-line
ART
or
were
simply
“taking
pills
elsewhere.”
Among
those
lost
to
follow-up,
a
significant
number
had
already
escalated
to
second-
or
third-line
therapy,
suggesting
that
even
patients
on
more
complex
treatment
plans
are
disengaging.
Several
back-to-care
records
explicitly
note
temporary
relocations
to
South
Africa,
Namibia,
or
other
clinics
elsewhere.
Mentions
of
“self-transfer”
and
taking
“pills
elsewhere”
recur
in
both
patient
groups,
underscoring
a
fragmented
landscape
in
which
patients
drift
between
public
and
private
providers.
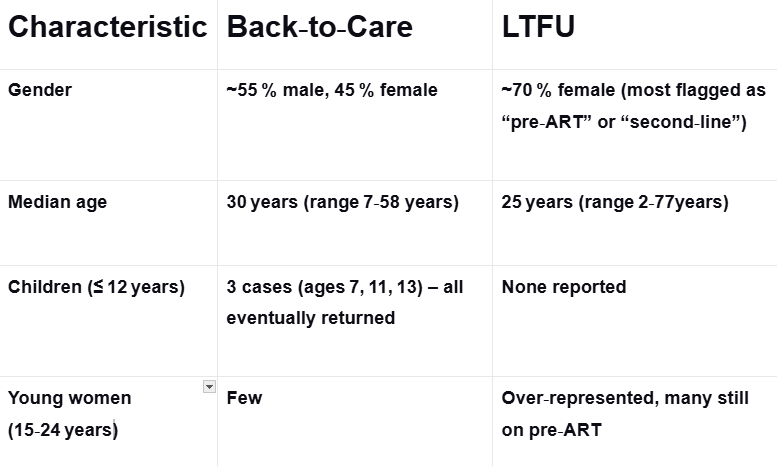
Children
appeared
only
among
the
back
to
care
returnees,
suggesting
that
caregivers
eventually
bring
them
back
to
care
after,
possibly
after
neglect,
periods
of
lack
of
awareness
or
guardian
change.
Young
women
dominate
the
LTFU
pool,
reflecting
socioeconomic
pressures,
including
transport
costs,
childcare
duties
and
the
need
to
earn
a
living,
which
pull
them
away
from
consistent
clinic
visits.
This
Mpilo
data
paints
a
complex
picture,
reflecting
that
short-term
treatment
gaps
can
often
be
corrected,
but
prolonged
disengagement
remains
a
persistent
challenge,
especially
among
vulnerable
populations.
The
data
also
shows
improved
data
systems,
patient
tracking
and
targeted
support
for
high-risk
groups
will
be
crucial
in
reducing
ART
default
and
improving
long-term
health
outcomes
in
Bulawayo.
Why
patients
default
In
interviews
as
to
why
people
default,
one
community
elder
in
Old
Lobengula,
Giyani
Moyo
said,
the
major
challenge
was
stigma.
“It’s
because
of
stigmatisation
at
the
point
of
collection
of
treatment
tablets.
It’s
how
staff
say
‘abe
TB
wozani
nga,
abe
HIV
yanini
le (TB
patients
come
here,
HIV
patients
go
there,’”
Moyo
said.
“At
clinics
it’s
prevalent,
worse
clinics
have
neighbours
and
friends
also
attending.”
A
medical
doctor
said
denial
is
another
major
reason
why
some
patients
default
on
treatment,
as
they
struggle
to
accept
their
diagnosis.
The
doctor,
who
requested
anonymity,
said
his
own
brother
was
diagnosed
with
HIV
in
2022
but
defaulted
on
medication
due
to
denial.
“In
2023,
my
brother
left
for
South
Africa,
where
his
condition
worsened.
We
later
received
a
phone
call
from
his
friends
informing
us
he
was
seriously
ill.
Since
I
am
the
doctor
in
the
family,
my
relatives
asked
me
to
go
and
talk
some
sense
into
him,”
he
said.
However,
when
he
arrived,
his
brother
refused
to
resume
treatment,
insisting
he
only
had isihlabo (pneumonia).
“Seeing
how
serious
his
condition
had
become,
I
arranged
for omalayitsha (cross-border
transporters) to
bring
him
back
home
by
force,”
he
explained.
The
brother
is
now
back
on
ART
and
picking
up.
Economic
hardships
and
Pill
Burden
Bulawayo
coordinator
for
Zimbos
Abantu,
which
runs two
mobile
clinics
in
Emganwini
and
Cowdray
Park, Charmaine
Dube,
who
has
worked
extensively
in
HIV
programming
with
various
stakeholders
in
the
district,
said
economic
hardship
and
social
realities
are
driving
many
patients
off
treatment.
“We
have
seen
a
lot
of
ART
patients
defaulting
on
their
medication.
Some
of
the
reasons
they
are
raising
are
pill
burden,
where
someone
just
gets
tired
of
taking
the
tablet
every
single
day,”
she
explained.
“Other
reasons
are
poverty,
where
people
are
struggling
to
make
ends
meet
and
to
put
food
on
the
table.
At
times,
a
person
will
prefer
not
to
take
the
tablet
than
to
take
it
on
an
empty
stomach.”
Dube
said
the
withdrawal
of
USAID
funding
has
also
exposed
serious
gaps
in
Zimbabwe’s
HIV
response,
particularly
in
urban
districts
disrupting
service
delivery
and
worsened
structural
barriers
already
facing
people
living
with
HIV.
“We
saw
some
facilities
that
were
offering
express
services
closing
down
and
people
being
referred
back
to
public
facilities,
where
there
are
longer
queues.
Most
of
the
people
are
self-employed
and
prefer
to
rather
go
hustle
than
spend
a
whole
day
queuing
for
their
medication.
That
has
resulted
in
many
defaulting,”
she
explained.
Health
system
constraints,
mobility
and
documentation
gaps
Staff
shortages
in
public
facilities
have
also
made
the
situation
worse.
“The
other
reasons
are
the
procedural
delays
people
face.
There
are
fewer
nurses,
so
it
takes
much
longer
for
a
person
to
be
attended
to.
Those
frustrations
are
causing
people
to
default
on
their
medication,”
Dube
said.
On
the
other
hand,
medical
staff
suggest
a
mix
of
economic,
social
and
psychological
drivers
behind
the
defaulting
trend.
Sister
in
charge
of
the
Opportunistic
Infections
(OI)
clinic
at
Mpilo
Hospital
Centre
of
Excellence,
Bongani
Khumalo,
says
the
centre
currently
serves
10
836
patients
on
ART.
“The
most
common
reasons
patients
give
for
defaulting
are
people
who
go
to
South
Africa
in
search
of
work
and
fail
to
get
medications
due
to
lack
of
legal
documents,
some
give
details
that
are
not
true,
their
phones
are
unavailable
or
it’s
a
wrong
number,”
he
said.
“Adolescents
struggle
with
adherence
despite
counselling,
pill
fatigue,
lack
of
disclosure
to
partners,
especially
in
new
relationships,
and
mental
health
issues.
Others
tell
you
they
had
no
transport
fare.”
From
his
observations,
the
crisis
has
a
youthful
face
and
also
cited
how
stigma
remains
a
persistent
factor.
“Some
youth
or
teenagers
have
been
taking
ART
for
their
whole
life
since
birth
and
are
now
fatigued,”
Khumalo
said.
Stigma
and
discrimination
Meanwhile,
some
patients
avoid
clinics
because
they
fear
being
recognised
by
neighbours,
said
Moyo,
the
community
leader.
Others
conceal
their
status
from
partners
and
families,
leading
to
hidden
struggles
with
adherence.
This
was
corroborated
by
National
AIDS
Council
(NAC)
provincial
manager,
Sinatra
Nyathi,
who
said
stigma
and
discrimination
continue
as
a
problem.
“We
do
have
the
stigma
index
report,
which
talks
about
where
we
are
in
terms
of
stigma
and
according
to
the
current
report,
we
are
not
going
down
in
terms
of
stigma,
but
actually
going
up,”
she
said.
A
2022
report,
the
Zimbabwe
People
Living
with
HIV
Stigma
Index
2.0,
revealed
that
despite
major
progress
in
HIV
treatment
access,
stigma
and
discrimination
remain
widespread.
The
study,
which
was
cross-sectional
and
conducted
in
all
Zimbabwe’s
10
provinces
with
1
400
participants
found
that
the
most
common
forms
of
discrimination
faced
by
people
living
with
HIV
(PLHIV)
include:
-
Exclusion
from
social
gatherings - Gossip
-
Verbal
abuse -
Physical
abuse
Stigma
was
reported
across
multiple
spaces,
including
families,
health
institutions
and
communities.
At
the
same
time,
the
report
indicated
Zimbabwe
has
made
remarkable
strides
in
treatment,
with
close
to
100
percent
of
respondents
reporting
access
to
HIV
care
services,
noting
strong
resilience
among
PLHIV,
which
is
vital
for
their
physical
and
psychological
well-being.
“Looking
into
the
future,
HIV
programming
in
Zimbabwe
should
prioritise
creating
an
enabling
environment
to
reduce
stigma
and
discrimination
against
PLHIV
to
sustain
and
enhance
their
health
outcomes
and
quality
of
life,”
the
report
concluded.
Danger
of
defaulting
The
NAC
provincial
manager
said
there
was
a
huge
danger
of
defaulting.
“You
need
to
understand
that
HIV
attaches
itself
to
your
T-helper
cells
in
order
to
infect
you.
If
that
attachment
doesn’t
happen,
infection
cannot
occur.
That’s
why
studies
have
shown
that
some
people
with
certain
cell
deformities
are
resistant
to
HIV,
it
simply
cannot
attach.
This
is
also
how
ARVs
work,”
Nyathi
said
“Different
ARVs
target
different
stages
of
the
HIV
life
cycle.
Some
prevent
attachment,
like
in
PEP,
which
is
given
soon
after
possible
exposure
to
stop
the
virus
from
entering
the
cells.
Others
target
multiplication
inside
the
cell,
preventing
the
virus
from
bursting
out
and
spreading.
These
drugs
are
specialised
to
fight
HIV.
That’s
why
we
use
a
combination
of
three
drugs
-to
block
HIV
at
multiple
points.
“If
you
stop
treatment,
you
give
the
virus
a
chance
to
multiply
quickly
and
attack
more
cells.
That’s
when
it
becomes
dangerous.
Many
people
stop
treatment,
feel
fine
for
a
while,
then
return
when
it’s
too
late.
The
virus
will
have
multiplied,
invaded
more
cells,
and
often
mutated.
HIV
mutates
very
fast,
and
once
it
changes,
the
drugs
you
were
taking
may
no
longer
be
effective.
“That
is
why
adherence
is
critical.
Staying
on
treatment
keeps
the
virus
suppressed
and
gives
you
a
much
better
chance
of
living
a
healthy
life.”
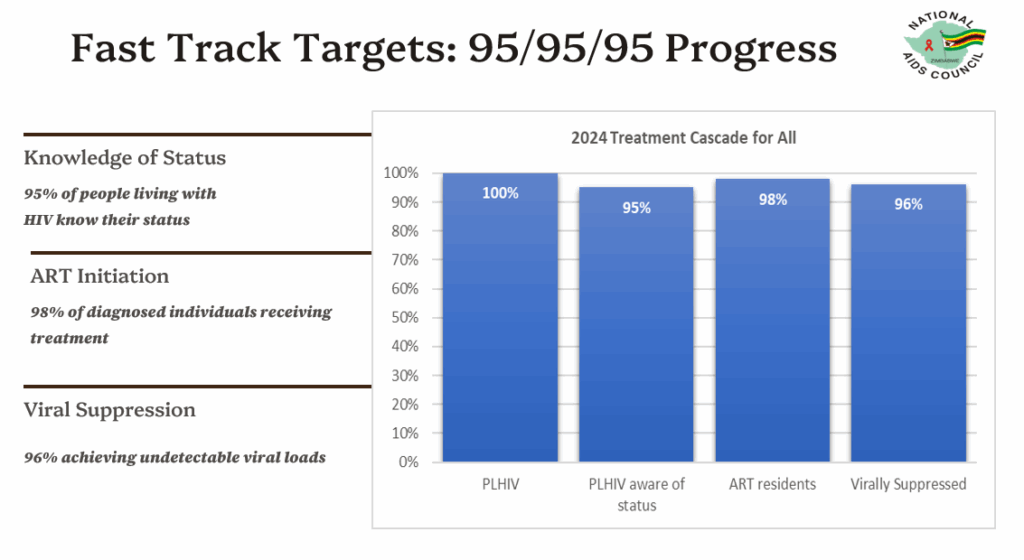
According
to
the
2025
HIV
Estimates
Report
for
Bulawayo
Metropolitan
province,
looking
at
the
treatment
progress,
95
percent
of
people
living
with
HIV
know
their
status,
98
percent
of
those
who
know
their
status
have
been
initiated
on
ART.
Among
those
on
ART,
96
percent
have
a
suppressed
viral
load.
Viral
suppression
remains
a
challenge,
largely
due
to
poor
adherence,
according
to
Mpilo
Hospital’s
Centre
of
Excellence
medical
director,
Dr
Nkazimulo
Tshuma.
Dr
Tshuma
said
starting
a
patient
on
ART
does
not
automatically
mean
their
viral
load
will
be
suppressed.
“We
can
give
one
medication,
but
it
is
now
up
to
the
patient
whether
they
take
it
properly
or
not.”
She
pointed
to
several
factors
that
contribute
to
inconsistent
medication
intake.
“There
are
issues
drug
to
drug
interruption
some
people
have
different
boxes
when
they
come
to
us
they
don’t
tell
us
they
have
other
conditions
and
we
wont
know
they
are
on
other
medications
so
ARvs
can
also
interrupt
with
other
medications
that
they
are
taking
causing
them
not
to
suppress
the
HIV
properly,
that
is
one
of
the
reason
why
people
are
not
suppressing
their
load,”
Dr
Tshuma
explained.
However,
Dr
Tshuma
stressed
that
the
main
reason
remains
poor
adherence.
“People
are
not
taking
medicine
properly
because
of
many
other
factors.
We
know
generally
we
are
all
undergoing
challenges
here
and
there,
some
people
when
they
go
through
challenges,
tend
to
stop
taking
medicines,”
she
said.
Dr
Tshuma
said
while
health
facilities
are
performing
well
in
terms
of
ART
supply
and
record-keeping,
achieving
viral
suppression
requires
more
than
providing
medication.
“So
medicines
are
being
supplied,
interestingly,
those
people
come
for
their
reviews,
monthly
or
every
six
months
or
they
collect
but
keep
them
at
home.
In
terms
of
us
supplying
ART
record
wise
we
would
have
done
very
well
but
come
to
viral
suppression,
sometimes
we
are
not
doing
so
well,”
she
said.

The
2025
HIV
Estimates
Report
for
Bulawayo
Metropolitan
Province
shows
that
the
city
continues
to
bear
a
significant
portion
of
the
national
burden
of
AIDS-related
deaths.
According
to
the
report,
approximately
946
people
living
with
HIV
in
Bulawayo
died
from
AIDS-related
causes
in
2024.
The
city’s
figures
represent
5.7
percent
of
Zimbabwe’s
total
16
723
AIDS-related
deaths
recorded
nationwide
during
the
same
period.
Adherence
push
Ward
26
Councillor
Mpumelelo
Moyo,
interviewed
at
a
mobile
clinic
in
Emganwini,
warned
that
men
who
default
on
HIV
and
TB
treatment
are
putting
their
own
lives
and
the
wellbeing
of
their
families
at
risk.
“Men
default
because
naturally
they
are
risk
takers,
but
where
they
take
risk
is
a
danger
to
their
lives,”
Moyo
said.
“They
should
be
continuously
educated
on
the
importance
of
taking
medication.
For
TB,
one
must
take
pills
until
the
course
is
completed,
and
for
HIV,
pills
are
taken
for
life.
Men
must
realise
it’s
their
health
that
is
at
risk,
and
stopping
treatment
could
leave
their
families
vulnerable.”
The
councillor
highlighted
his
role
in
encouraging
adherence.
“It
is
my
responsibility
as
a
councillor
to
encourage
men
wherever
I
go
to
take
pills
continuously,
not
to
default
and
be
there
for
their
families,”
he
said.
The
PMD,
Dr
Siamuchembu
also
warned
on
how
defaulting
is
a
“big
problem”
particularly
for
TB.
“If
I
am
on
treatment
and
default,
I
develop
TB
resistance,
which
I
can
give
to
you.
The
person
infected
doesn’t
have
to
do
anything
but
just
has
to
be
close
to
me
to
get
TB.
We
then
end
up
spreading
a
drug-resistant
TB,
which
we
can’t
afford.
This
is
a
problem
for
the
country
because
we
will
not
be
able
to
contain
it,”
he
said.
“We
want
to
treat
everyone
whom
we
can
treat,
cure
them
and
make
sure
they
don’t
spread
it.
It’s
the
same
thing
with
HIV,
except
that
with
HIV
most
of
the
time
you
have
to
consent
to
have
sex
and
to
get
it.
But
with
TB,
you
don’t
have
to
do
anything
but
be
close
to
a
person
with
TB.
Even
if
you
don’t
know,
you’ll
get
it.
You
see
that?
We
want
to
cut
those
numbers
down.
We
want
to
get
rid
of
TB
and
HIV,
as
public
health
concerns
by
the
year
2030.
We
only
have
less
than
five
years
to
do
this.
So
we
want
to
accelerate
that.”
Emerging
solutions
As
a
response,
hospital
staff
at
Mpilo
said
they
are
updating
record
keeping
systems
and
the
rollout
of
an
electronic
health-record
(EHR)
platform
is
expected
to
improve
tracking
across
facilities,
flag
duplicate
prescriptions
and
support
patient
retention
for
those
who
move
between
clinics.
Health
authorities
said
they
were
also
pushing
differentiated
service
delivery
(DSD)
models
to
reduce
barriers
but
this
has
been
affected
by
the
foreign
aid
funding
cuts.
Under
this
model,
families
were
allowed
to
send
one
member
to
collect
ART
for
everyone.
In
some
rural
areas,
patients
linked
to
Community
ART
Refill
Groups
(CARGS)
took
turns
collecting
for
each
other.
In
cross-border
communities,
the malayitsha system
evolved
where
these
informal
transporters
ferry
both
goods
and
medical
records
between
Zimbabwe
and
South
Africa,
collecting
ART
on
behalf
of
patients
working
in
the
diaspora.
“The malayitsha is
also
taught
how
to
maintain
those
drugs,
make
sure
they
are
packaged
well.
It’s
very
safe,”
Nyathi
said.
NAC
Programmes
Officer,
Douglas
Moyo,
said
the
fact
that omalayitsha were
organising
themselves
and
taking
turns
to
collect
medication
shows
real
commitment.
“They
have
sustained
that
arrangement
for
a
long
time.
If
you
want
to
see
the
success
of
the omalayitsha system,
go
to
Tsholotsho
rural
clinics.
Most
of
their
clients
are
actually
in
Botswana
and
South
Africa,
not
in
the
villages.
It’s
a
very
successful
model,
though
not
well
documented
and
it’s
proving
to
be
very
effective
in
rural
areas,
even
in
places
like
Plumtree.”
Despite
these
innovations,
staff
acknowledge
gaps
and
funding
challenges.
Follow-up
systems
often
fail
once
patients
give
false
addresses
and
mental
health
services
remain
thinly
stretched,
leaving
many
untreated
for
depression
and
substance
abuse,
both
linked
to
defaulting.
Khumalo
said
the
OI
clinic
tries
to
cushion
patients
with
support
groups,
peer
counselling,
telehealth,
free
lab
services
and
even
cervical
cancer
screening.
“To
keep
patients
on
ART
we
must
provide
individualised
care,
address
client
concerns,
and
monitor
progress,”
said
the
sister
in
charge.
The
coordinator
for
Zimbos
Abantu
Bulawayo,
concurred
community
engagement
and
support
groups
are
critical
in
keeping
patients
on
track.
“There
should
be
strategies
like
community
support
groups,
where
people
are
encouraged
and
empowered
to
take
up
their
health
more
seriously,”
Dube
explained.
“Traditional
methods
where
people
have
been
grouped
in
groups
of
10
or
20,
maybe
it’s
an
ART
or
TB
support
group
where
those
recipients
of
care,
share
experiences
of
what
they
are
facing
and
how
they
are
tackling
challenges
and
encourage
each
other
to
continue
taking
up
health
education
also
work.”
Dube
also
highlighted
the
importance
of
addressing
nutritional
challenges
that
often
affect
adherence.
“We
have
also
opted
that
people
don’t
focus
on
the
most
expensive
food
but
the
basics
like umfushwa,
which
is
more
accessible,”
she
said,
adding
that
“growing
gardens
at
the
back
of
their
homes
so
they
get
something
to
eat
as
much
as
they
are
facing
economic
challenges,”
helps
people
stay
on
treatment
without
compromising
their
health.