Bulawayo
National
AIDS
Council
(NAC)
Programmes
Officer,
Douglas
Moyo
said
the
city
was
witnessing
patterns
that
pointed
to
persistent
risky
sexual
behaviour,
weak
behaviour
change,
and
heightened
vulnerability
to
HIV
infection.
Moyo
said
STIs
remained
a
critical
public
health
issue
because
of
their
direct
link
to
HIV
transmission.
“The
topical
issue
now
of
sexually
transmitted
infections
STIs.
HIV
is
transmitted
easily
when
one
has
a
sexually
transmitted
infection.
Why?
Because
sexually
transmitted
infections
would
provide
easy
passage
through
the
breaking
of
the
skin.
Such
that
there
is
an
easy
entry,”
he
said
to
the
media
recently
while
giving
the
latest
Bulawayo
HIV
Programmes
Update.
Moyo
explained
that
infections
such
as
syphilis,
gonorrhoea
and
chlamydia
significantly
increase
susceptibility
to
HIV
and
act
as
markers
of
high-risk
sexual
behaviour.
“If
you
walk
into
any
health
facility,
be
it
a
private
doctor
or
a
clinic
with
an
STI.
This
is
clear
evidence
that
‘here
is
somebody
who
exposed
themselves
through
having
condomless
sex
or
who
had
an
accident
somehow
during
the
sexual
encounter,’”
Moyo
said.
Drawing
parallels
with
pregnancy,
Moyo
said
STIs
and
PMTCT
data
both
point
to
unprotected
sex.
“Just
like
somebody
who
walks
into
a
facility,
they
are
pregnant,
it’s
evidence
that
they
had
unprotected
sex,
isn’t
it?
Because
there
is
no
way
they
could
get
pregnant
if
they
were
protected.
So
those
two,
PMDCT
and
STI,
are
key
evidence
of
unprotected
sexual
intercourse.
But
the
one
that
we
are
most
worried
about
is
this
one
-Sexually
transmitted
infections,”
he
said.
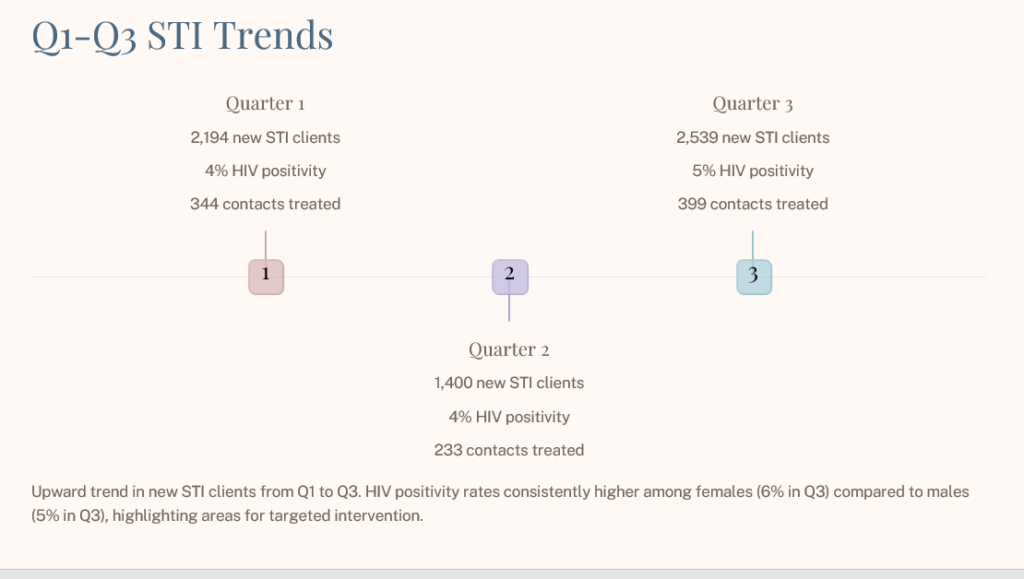

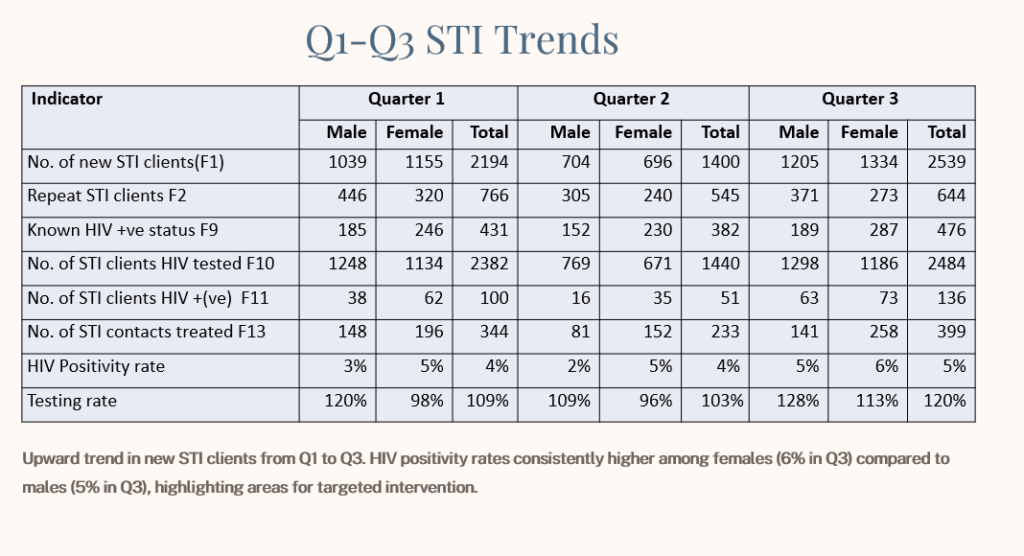
Data
from
the
first
three
quarters
of
the
year
shows
a
troubling
upward
trend.
In
the
first
quarter
alone,
Bulawayo
recorded
2
194
new
STI
cases.
“Look
at
the
trend.
Look
at
what
happened
in
the
first
quarter.
Quarter
one,
we
had
2
194
new
cases
underline
the
word
new
and
a
quarter
has
only
three
months.
In
just
three
months,
we
recorded
2
194
STI
cases,”
Moyo
said.
He
said
all
STI
patients
are
routinely
tested
for
HIV,
with
the
data
revealing
persistent
HIV
positivity
among
those
presenting
with
STIs.
“And
then
the
management
protocol
now
for
STIs
is
that
anyone
who
presents
with
an
STI
should
be
tested
for
HIV.
then
we
can
see
the
positivity
rate
was
4
percent,”
he
said.
Although
the
number
of
new
STI
cases
declined
in
the
second
quarter
to
about
1
400,
Moyo
cautioned
against
celebrating
the
drop
without
deeper
analysis.
“Quarter
two,
the
number
declined.
But
that
decline
needs
to
be
investigated,
to
say,
was
it
a
genuine
or
real
decline,
or
is
there
something
that
happened
with
the
data
capturing?
Because
a
decline
from
that
to
that,
yeah,
we
need
to
find
out,”
he
said.
“We
need
to
find
reasons
if
there
were
programmes,
awareness
sessions,
or
activities
that
resulted
in
that
decline.
We
need
to
find
out
and
celebrate
those
approaches
because
they
did
wonders
but
look
at
the
positivity
rate,
again,
it
remained
at
four
percent
HIV
positivity
in
the
second
quarter
and
we
are
talking
about
new
cases.”
By
the
third
quarter,
new
STI
cases
had
surged
again
to
2
539,
reinforcing
concerns
that
Bulawayo
was
not
making
sustained
progress.
“Then
look
at
the
last
quarter,
which
is
now,
the
previous
quarter,
the
quarter
three.
We
had
2
539
new
STI
cases,”
Moyo
said.
Moyo
said
when
the
first
and
third
quarters
are
compared,
the
overall
direction
is
clearly
upward.
“When
you
look
at
the
trend,
if
we
are
making
any
progress,
look
at
the
number
in
quarter
one
and
compare
it
with
quarter
three,
it’s
going
up.
Don’t
worry
about
the
decline
in
the
second
quarter.
If
you
were
to
draw
a
trend
line
of
a
graph,
it
would
be
going
up,”
he
said.
“So
if
you
were
to
draw
a
trend
line
from
there,
it
would
go
down
and
then
shoot
up
like
that.
That
is
a
cause
for
concern,”
Moyo
added.
He
stressed
that
STI
cases
also
signal
active
sexual
networks,
increasing
the
risk
of
wider
HIV
transmission.
“Remember,
for
anyone
who
presents
with
a
sexually
transmitted
infection,
it’s
clear
evidence
that
they’re
in
a
sexual
network.
How
wide
that
sexual
network
is,
no
one
knows,”
he
said.
“So
it
is
a
cause
for
concern
if
we
continue
to
get
2
539
new
cases
by
the
end
of
last
quarter,”
Moyo
said.
Moyo
said
the
persistently
high
HIV
positivity
rates
among
STI
patients
show
that
HIV
remains
a
serious
threat.
“Somebody
asked
a
question
in
one
of
the
groups
that
is
HIV
still
a
threat?
I
think
this
is
evidence
to
show
that
HIV
is
still
a
threat.
If
you
can
have
a
positive
rate
of
four
percent
and
it
goes
up
to
five
percent,”
he
said.
He
said
fourth-quarter
data
was
still
being
compiled
and
analysed.
“We
are
yet
to
analyse
data
for
the
fourth
quarter
because
the
year
has
not
ended.
December,
I
think,
we
are
finishing
our
data
collection
next
week.
This
is
when
we
will
analyse
and
see
what
this
data
is
going
to
show
us
in
the
fourth
quarter,”
Moyo
said.
Beyond
new
infections,
Moyo
said
repeat
STI
cases
were
one
of
the
most
troubling
indicators,
showing
limited
behaviour
change.
“Look
at
the
repeat
STIs,
which
is
a
cause
for
concern.
When
we
talk
about
the
repeat,
we
are
talking
about
those
people
who
are
presenting
to
a
facility,
not
for
the
first
time
at
the
STI,”
he
said.
Among
males,
repeat
infections
remained
high
across
all
three
quarters.
“For
males,
I
mean
in
the
first
quarter
we
had
766
repeat
cases.
In
the
second
quarter
we
had
545.
And
then
in
the
third
quarter,
644
repeat
STIs,
which
show
that
people
are
not
changing
their
behaviour,”
Moyo
said.
He
said
repeat
infections
often
result
from
failure
to
treat
sexual
partners
and
poor
communication
within
relationships.
“A
change
of
behaviour
could
mean
that
you
have
an
STI.
You
have
challenges
or
fears
of
approaching
your
significant
other.
You
go
and
seek
treatment
clandestinely
or
privately,
you
get
treated.
But
then
you
come
back
and
get
re-infected
from
the
same
partner
because
you
didn’t
discuss
these
issues,”
he
said.
Moyo
emphasised
the
importance
of
partner
notification
and
contact
tracing.
“So
when
it
comes
to
STIs,
it
is
very
important
for
sexual
partners
to
be
treated.
Hence
that
programme
of
tracing
the
contact,”
he
said.
He
said
tracing
sexual
networks
is
critical
to
breaking
cycles
of
reinfection.
“Then
the
sexual
partner
will
be
followed
up.
Then
that
other
partner
will
be
asked
‘who
is
your
other
sexual
partner.’
So
the
whole
network
should
be
followed
up
and
be
brought
to
treatment,”
Moyo
said.
The
high
number
of
repeat
cases,
he
said,
points
to
persistent
risk-taking
and
low
self-perceived
vulnerability.
“So
the
repeat
cases,
the
repeats
are
a
challenge.
They
are
showing
us
that
some
people
are
not
changing
their
behaviour.
Some
people
still
don’t
perceive
themselves
as
at
risk
of
infection,”
he
said.
Moyo
warned
that
this
behaviour
significantly
increases
the
risk
of
HIV
transmission.
“So
if
they
can
get
repeat
STI
cases,
what
about
the
exposure
or
the
risk
of
contracting
HIV?
It
is
heightened
isn’t
it?”
he
said.
Post
published
in:
Featured